Origin: The New England Journal of Medicine, January 4, 2024
Original Article Title: Drug-Eluting Resorbable Scaffold versus Angioplasty for Infrapopliteal Artery Disease
What is a Drug-Eluting Resorbable Scaffold?
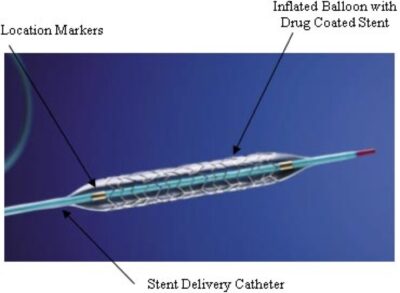
Drug-Eluting Resorbable Scaffolds (DERS) represent a significant advancement over traditional metal stents. Constructed from biodegradable materials, DERSs serve the critical function of maintaining arterial patency but do so temporarily. Over time, they dissolve or are metabolized by the body, which can diminish the long-term risks commonly associated with permanent stents.
The composition of DERS involves bioresorbable polymers that allow them to integrate seamlessly with bodily processes, eventually disappearing once their structural support is no longer necessary. Additionally, these scaffolds are imbued with pharmacological agents, similar to traditional drug-eluting stents. These medications are released gradually to prevent restenosis, which is the re-narrowing of the artery due to cell proliferation at the treatment site.
This technology underscores a pivotal shift towards interventions that not only provide immediate therapeutic benefits but also align with the body’s natural healing mechanisms, enhancing long-term cardiovascular health outcomes.
What is Angioplasty for Infrapopliteal Artery Disease?
This minimally invasive procedure targets the arteries below the knee, which are crucial for blood supply to the lower leg and foot. In cases of peripheral artery disease (PAD), these arteries may become narrowed or blocked, leading to severe complications such as chronic pain, ulcers, and even the risk of limb amputation.
The angioplasty procedure for infrapopliteal artery disease involves several key steps. Initially, access is gained through a small incision, typically in the groin area, to introduce a catheter into the artery. This catheter is then meticulously guided to the site of the blockage. Upon reaching the target area, a small balloon attached to the tip of the catheter is inflated. This inflation compresses the plaque against the artery walls, effectively widening the artery and restoring essential blood flow.
In certain scenarios, a stent—a small wire mesh tube—may also be deployed to keep the artery open. While stenting is a common practice in the treatment of coronary and carotid artery diseases, its application in infrapopliteal arteries is considered more selectively. The decision to place a stent depends on the patient’s specific condition and the severity of the arterial blockage.
This procedure not only mitigates the immediate risks associated with PAD but also plays a crucial role in the long-term management of the disease, aiming to improve patient quality of life and prevent more severe outcomes.
What is Interesting about this Article?
Peripheral artery disease (PAD) remains a pressing health issue globally, affecting approximately 230 million people worldwide, including between 7 to 12 million in the United States. PAD leads to the narrowing or blockage of arteries, escalating to chronic limb-threatening ischemia—a critical condition that could culminate in tissue loss or amputation if not effectively addressed. Angioplasty traditionally has been utilized to manage such severe arterial conditions. However, this treatment is frequently accompanied by the need for repeated interventions due to complications such as restenosis, where the artery narrows once more after treatment.
In response to these ongoing challenges, innovative treatments have been developed to enhance patient outcomes. One notable advancement is the introduction of the drug-eluting resorbable scaffold, a device designed to temporarily support the artery while releasing everolimus, a drug that inhibits restenosis. A pivotal study demonstrated that this approach is superior to traditional angioplasty for patients with infrapopliteal artery disease. The scaffold provides structural support until the artery can sustain itself and gradually dissolves within the body, minimizing the risk of the long-term complications often associated with permanent stents. These results signify a substantial progression in PAD treatment, offering a more effective and potentially safer alternative to conventional angioplasty, particularly for those facing chronic limb-threatening scenarios.
JournalDoc Notes
Untreated limb-threatening ischemia in the legs presents a severe health challenge, marked by persistent pain, a high incidence of ulceration, gangrene, and a substantial risk of amputation. These dire consequences highlight the need for effective intervention strategies. In an insightful editorial, Dr. Joshua A. Beckman suggests that the management of PAD is evolving significantly with the advent of device therapy, particularly through the use of resorbable scaffolds. These innovative devices are designed to provide temporary support to the vessel wall, crucially preventing both acute and subacute vessel closures, thereby advancing the treatment landscape of PAD.
This evolving approach was the focus of a recent study that examined not only the mechanical success of the device but also the clinical outcomes for the patients. Such research underscores the fundamental principles of evidence-based medicine, which relies heavily on tangible clinical benefits to validate medical practices. The study’s emphasis on both device efficacy and patient-centric outcomes serves as a robust model for future research. It suggests that subsequent studies in this field should continue to integrate clinical outcomes to fully assess the effectiveness and safety of new technologies in real-world scenarios, ensuring that advancements in medical devices translate into meaningful health benefits for patients with PAD.
CLICK HERE FOR MORE INFORMATION ON THIS STUDY
Disclaimer: The Article of the Week selections made by JournalDoc physicians are independent and unbiased, with no commercial conflicts of interest. JournalDoc neither supports nor endorses the opinions or findings presented in the articles. The conclusions drawn in these articles may require further validation through additional research and expert consensus.
